Care Solutions Help Prevent High-Cost Claims From Escalating
Fragmented care triggers avoidable costs and more outcomes.
Trusted clinical results you can count on
Guide members to the right care, every time
Reduce unneccesary utilization without denying care

22% ▾
inpatient days
32%
reduction in total cost of care

High-cost claims escalate fast. Guide members before costs spike.
Nurse-led care management and fast pre-certifications keep care moving, reduce avoidable utilization, and steer members to cost-effective providers.

Your ally for smarter, patient-centered care
An in-house clinical team delivers integrated services to coordinate care, remove delays, and connect members to the right providers when it matters most.
Fast approvals that help keep care moving
Member-friendly pre-certifications reduce delays, support timely treatment, and help prevent avoidable escalation.
Fast turn-around
Same-day to 2–3 business day approvals versus a 10-day industry average
Fewer approval delays
Missing information is resolved proactively to help keep approvals on track
Partner-first approach
We work with providers to support timely care rather than creating extra friction

Nurse-led guidance through serious illness or injury
Dedicated nurse support helps members navigate complex care needs with clearer guidance, coordination, and follow-through.
Personal clinical guidance
Nurse-led support helps members understand next steps and stay on track through care
Complex care coordination
Support across serious illness or injury helps reduce confusion and prevent delays
Smoother care transitions
Better coordination helps reduce gaps when care moves across providers and settings
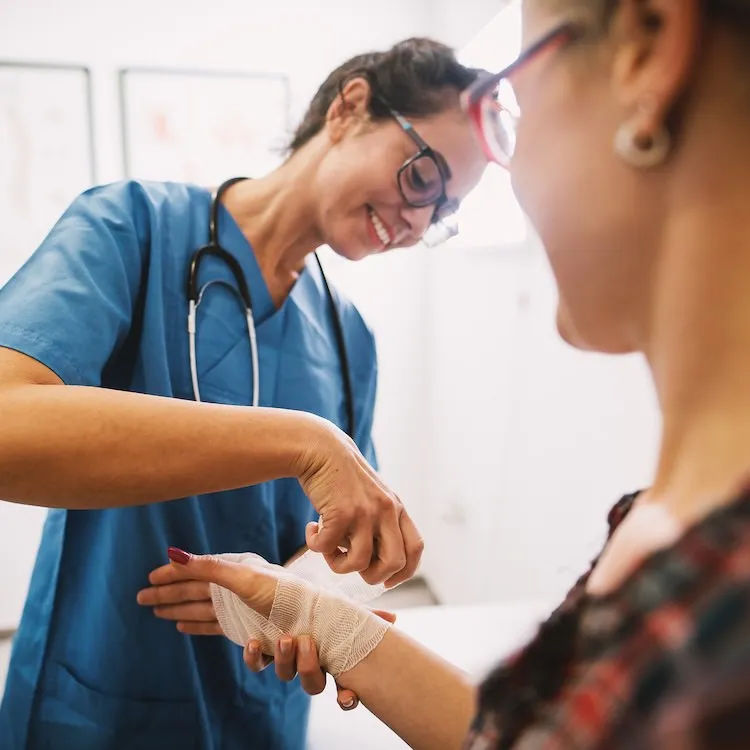
Navigation strategies that direct members to the right care at the right time and the right place
Help members choose high-value providers and clinically appropriate settings of care through structured pathways that reduce unnecessary spend and improve outcomes.
Evidence based direction
Use clinical rules and high value provider data to guide members toward the safest and most cost-effective care options
Proactive outreach
Identify members at key decision points and provide timely guidance that helps them avoid low-value or high-cost care
Integrated support
Align nurses, care navigators, and digital tools to deliver consistent guidance through every step of the member journey

What are Care Solutions?
Care Solutions are services that help members get to the right care sooner through pre-certifications, care management, and guided care support. They reduce delays, improve coordination, and help prevent high-cost claims from escalating in self-funded health plans.
How OneVeracity operates
Each solution is supported by simple implementation, hands-on account management, responsive member support, and reporting that keeps progress visible.
Implementation
Quick implementation that is seamless and reliable
Account management
End-to-end support across billing, eligibility, claims, renewals, and open enrollment to ensure your benefits program runs smoothly
Member support
Proactive, high-touch member support that resolves issues early, guides members to the right care, and manages escalations with fast, informed intervention
Reporting
Actionable reporting and financial analysis that support informed decision-making and long-term cost management

What is self-funded healthcare?
Self-funded healthcare is a model where employers pay employee healthcare claims directly instead of purchasing a traditional insurance plan. Employers gain more control over plan design, costs, and reporting, while OneVeracity helps support administration, risk protection, and cost control.
Earlier guidance. Better coordination. Stronger outcomes.
Care Solutions combine proactive support, earlier intervention, and data-driven insights to help members get to the right care before costs and complexity escalate
Prevention-focused support
A proactive approach helps guide members before health challenges escalate
Early needs identification
Data-driven insights help identify needs earlier and support faster intervention
Personalized health coaching
Personalized coaching and support go beyond traditional disease management
Faster pre-certifications
Member-friendly approvals help reduce delays and keep care moving
Nurse-led care management
Dedicated nurse support helps members navigate serious illness or injury
Coordinated care transitions
Seamless coordination across providers and services supports timely care
Right-care navigation
Members are guided to the right care and cost-effective providers earlier
Measurable clinical impact
Better transitions, fewer delays, and healthier outcomes support lower total cost
Real results.
Real partnerships.
Real self-funded employers and brokers. Clear savings drivers.
Proof your team can review, defend, and act on.

Questions? Answers.
Your most frequently asked questions, all in one place. If you don’t see what you need, book a call here.
How do Care Solutions reduce healthcare costs for self-funded employers?
Care Solutions reduce costs by guiding members through complex care needs, tightening utilization decisions, and preventing high-cost claims from escalating. Fragmented care can trigger avoidable costs and poor outcomes when members face delays, unnecessary ER visits, or gaps in transitions. OneVeracity’s Care Solutions provide support that keeps care moving, reduces avoidable ER utilization, and connects members to cost-effective, high-performing providers when it matters most. Services include pre-certifications, nurse-led care management, and guided care pathways with proactive outreach. The impact is measured through utilization and cost outcomes, including fewer avoidable ER visits and admissions, better care transitions, and reduced readmissions. One national client reported 456% ROI after adopting OneVeracity’s Care Solutions and other integrated programs.


What services are included in Care Solutions for self-funded health plans?
Care Solutions delivers three core services that reduce delays, minimize waste, and improve outcomes across complex care. First, Pre-certifications provide fast, member-friendly approvals, typically 2-3 days versus a 10-day industry average. Second, nurse-led Care Management provides consistent guidance through serious illness or injury, helping members navigate treatment decisions and coordination. Third, Guided Care Pathways provide proactive, data-driven coaching, access to virtual specialty care, early intervention, and nationwide access to top-performing, cost-effective providers. Together, these services reduce avoidable utilization and help prevent escalation in high-cost claims. The approach is designed to work with existing plan arrangements while also providing account management, member support, and reporting that improve outcomes and cost control.


How quickly can Care Solutions support high-cost cases and approvals?
Care Solutions are designed to reduce avoidable delays that often drive cost and member frustration in complex care. A key service is pre-certifications with faster, member-friendly approvals, typically 2-3 days compared to a 10-day industry average. That speed matters because delays can lead to missed care windows, avoidable ER use, and cost escalation. Care Solutions also include nurse care managers who can engage members quickly, coordinate across providers, home health, caregivers, and community resources, and help keep care plans moving. The goal is timely decisions and coordinated support so members get to appropriate care sooner and clients see fewer gaps, fewer avoidable utilization events, and cleaner continuity of care.


How are Care Solutions different from traditional case management?
Traditional case management can be reactive, engaging after costs have already escalated or after members have struggled through delays and fragmented handoffs. Care Solutions are designed to intervene earlier, keep care moving, and guide members through decisions that drive both outcomes and cost. The service mix combines faster pre-certifications, nurse-led guidance through serious illness or injury, and proactive guided pathways that connect members to cost-effective, high-performing providers. The result is fewer delays, fewer avoidable utilization events, and better care transitions. Services can be delivered standalone or bundled based on need, with a focus on clear support and measurable impact rather than broad promises.


Do Care Solutions replace carriers, vendors, or existing clinical resources?
Care Solutions are designed to work alongside existing carriers, vendors, and clinical resources by adding coordinated support where fragmentation typically creates cost and outcomes risk. The goal is not to replace what is already in place, but to reduce gaps in navigation, approvals, and complex-case coordination so members get timely guidance and care plans stay on track. Care Solutions support coordination across providers and care settings, including home health, caregivers, and community resources, which helps reduce delays and improve continuity. This approach lets clients strengthen utilization control and member experience without forcing a rip-and-replace change, while keeping results measurable.


How do Care Solutions measure impact without overpromising outcomes?
Care Solutions measure impact using clear utilization and outcome metrics tied to avoidable cost drivers. Examples include reductions in avoidable ER visits and admissions, more efficient care transitions that reduce gaps and delays, decreased readmissions, improved chronic condition control, and reductions in inpatient days, admits, and PMPM total medical spend. These measures connect care coordination to both member experience and total plan cost. Clients also get reporting with actionable insights so they can see what is happening, understand why it matters, and adjust priorities over time. One national client reported 456% ROI after adopting OneVeracity’s Care Solutions and other integrated programs. Other clients have also seen a 22% reduction in inpatient days, a 14% reduction in admits, and a 32% reduction in PMPM total medical spend.



Practical thinking for
better healthcare
Straightforward resources for renewal conversations, leadership reviews, and day-to-day plan decisions

Schedule a strategy review today
Tell us what’s driving your clients’ renewal increases. We’ll show where spend is leaking, which levers will move it fastest, and how to roll out change with minimal disruption.
Thank you!
Your request has been received. A member of our team will reach out shortly to follow up.























